Posted By Dr Ajay Bahadur | Cardiologist in Lucknow
Fasting has become one of the most popular health trends worldwide. From Intermittent Fasting (IF) to religious fasting during Ramadan or Navratri, millions of people skip meals to lose weight, improve brain health, or detoxify their bodies. But for someone living with a heart condition, the question isn’t just about weight loss—it’s about safety.
Is fasting safe for heart patients? The answer isn’t a simple “yes” or “no.” It depends on your specific condition, the medications you take, and how you approach the fast.
In this detailed guide, we will explore the benefits, risks, and essential precautions for fasting with heart disease. If you are seeking expert advice, consulting a professional like Dr. Ajay Bahadur, a renowned Cardiologist in Lucknow, is the first step before changing your eating habits.
Understanding Fasting: What Is It?

At its simplest, fasting means going without food (and sometimes water) for a specific period. There are several ways people fast today:
-
Intermittent Fasting (16/8): You eat during an 8-hour window and fast for 16 hours.
-
24-Hour Fasts: Eating once a day.
-
Water Fasting: Consuming only water for a day or more.
-
Religious Fasting: Avoiding certain foods or all food/drink from sunrise to sunset.
While these methods offer various health perks, the heart is a sensitive organ that requires a steady balance of minerals and energy to pump blood effectively.
The Benefits of Fasting for Heart Health

For a person with a healthy heart or someone at risk of heart disease (but not yet diagnosed with a severe condition), fasting can offer several “cardio-protective” benefits:
-
Weight Management: Obesity is a leading cause of heart attacks. Fasting helps reduce calorie intake.
-
Lower Blood Pressure: Some studies show that intermittent fasting can help reduce systolic and diastolic blood pressure.
-
Improved Cholesterol: Fasting can lower LDL (bad cholesterol) and triglycerides while potentially raising HDL (good cholesterol).
-
Reduced Inflammation: Chronic inflammation is a silent killer for the heart. Fasting helps the body reduce inflammatory markers.
-
Insulin Sensitivity: By giving the pancreas a break, fasting helps the body manage blood sugar better, which protects the blood vessels.
However, if you already have a diagnosed heart condition, these benefits must be weighed against significant risks.
The Risks: Why Heart Patients Must Be Cautious
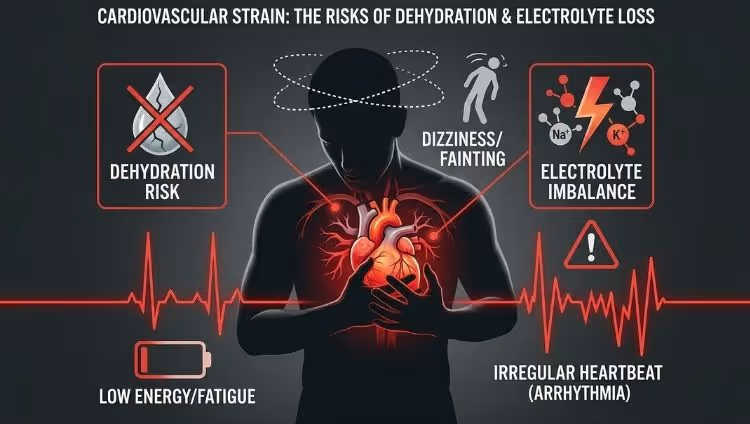
The heart works 24/7. It doesn’t get a break even when you are sleeping or fasting. When you stop eating, several things happen in your body that can trigger heart issues:
1. Electrolyte Imbalance
Your heart beats because of electrical signals. These signals rely on minerals called electrolytes—specifically Potassium, Magnesium, and Sodium. Fasting, especially water fasting, can cause these levels to drop. An imbalance can lead to Arrhythmia (irregular heartbeat), which can be fatal for heart patients.
2. Dehydration
Many people forget to drink enough water while fasting. Dehydration makes the blood thicker, forcing the heart to work harder to pump it. This increases the risk of blood clots and puts extra stress on the heart muscles.
3. Medication Complications
Most heart patients take medications like blood thinners, beta-blockers, or diuretics (water pills). Many of these drugs must be taken with food to prevent stomach irritation or to ensure proper absorption. Taking a diuretic while fasting can lead to severe dehydration and kidney strain.
4. Blood Sugar Swings
If a heart patient also has diabetes, fasting can cause “hypoglycemia” (dangerously low blood sugar). Low blood sugar can trigger a rapid heart rate and put immense stress on the cardiovascular system.
Chart: Fasting Types and Safety Levels for Heart Patients
To help you understand the risks, here is a quick comparison chart:
| Fasting Type | Description | Safety Level for Heart Patients | Key Concern |
| Intermittent (16:8) | Fast for 16 hours, eat for 8 | Moderate | Timing of heart medications. |
| 24-Hour Fast | No food for a full day | High Risk | Sudden drop in electrolytes/BP. |
| Water Fasting | Only water for 24+ hours | Very Dangerous | Severe mineral loss & heart strain. |
| Religious Fasting | No food/water (Sunrise-Sunset) | Moderate to High | Dehydration and “re-feeding” stress. |
| Fruit Fasting | Only eating fruits | Low to Moderate | High sugar intake/Insulin spikes. |
Note: Always consult Dr. Ajay Bahadur, a leading Heart Doctor in Lucknow, before attempting any of these.
Heart Conditions and Fasting: A Specific Look
Not all heart conditions are the same. Your ability to fast depends on what part of your heart is affected.
Heart Failure
Patients with Congestive Heart Failure (CHF) often have strict fluid restrictions. Fasting can disrupt the delicate balance of fluids and salts in their bodies. If you have CHF, long-term fasting is generally not recommended.
Atrial Fibrillation (AFib)
AFib is an irregular heart rhythm. Because AFib is highly sensitive to electrolyte changes (especially potassium and magnesium), fasting can trigger an episode. If you have AFib, you must be extremely careful and monitor your mineral intake.
Post-Surgery or Post-Stent
If you have recently had a bypass surgery or a stent placement, your body needs constant nutrition to heal the tissues. Fasting during the recovery phase (the first 6–12 months) is usually discouraged by experts like Dr. Ajay Bahadur.
Hypertension (High Blood Pressure)
Patients with high blood pressure often see improvements with intermittent fasting. However, the danger lies in the “Re-feeding Syndrome.” If you break a fast with a high-salt or high-carb meal, your blood pressure can spike dangerously high.
Expert Advice from Dr. Ajay Bahadur (Heart Doctor in Lucknow)
When dealing with the heart, there is no “one size fits all” approach. According to Dr. Ajay Bahadur, a top Heart Doctor in Lucknow, the most important factor is Medical Supervision.
Dr. Bahadur emphasizes that heart patients should never stop their medications to accommodate a fast. If a patient wants to fast for religious or health reasons, the medication schedule must be adjusted by a cardiologist. For example, some blood pressure medications might need to be reduced during a fast to prevent the blood pressure from dropping too low (hypotension).
If you are in Lucknow and planning a lifestyle change involving fasting, visiting a specialist like Dr. Ajay Bahadur ensures that your heart is monitored through ECGs or blood tests to check if your body can handle the stress of fasting.
How to Fast Safely If You Have a Heart Condition

If your doctor gives you the “green light” to try a mild form of fasting (like the 16:8 method), follow these safety steps:
-
Stay Hydrated: Drink plenty of water during the fasting hours. If your fast allows, herbal tea or lemon water (without sugar) can help.
-
Focus on Electrolytes: Ensure your “eating window” includes foods rich in potassium (bananas, spinach) and magnesium (nuts, seeds).
-
Break the Fast Gently: Do not eat a massive, greasy meal immediately. Start with a light soup or a small portion of protein to avoid stressing the heart.
-
Monitor Your Body: Use a home blood pressure monitor and a pulse oximeter. If your heart rate goes above 100 bpm or your BP drops significantly, stop the fast immediately.
-
Don’t “Dry Fast”: Heart patients should never fast without water. Dehydration is the quickest way to end up in the emergency room.
Warning Signs: When to Stop Fasting Immediately
If you are fasting and experience any of the following, eat something small and call your doctor right away:
-
Dizziness or Lightheadedness: This could mean your blood pressure is too low.
-
Palpitations: Feeling like your heart is “fluttering” or skipping a beat.
-
Extreme Fatigue: If you feel too weak to walk across the room.
-
Chest Pain: Any discomfort in the chest area is a red flag.
-
Cold Sweats: This could be a sign of a sudden drop in blood sugar or heart distress.
The Role of Diet in Fasting
What you eat during your non-fasting hours is just as important as the fast itself. A heart patient’s diet should be:
-
Low in Sodium: Excess salt causes water retention and high BP.
-
High in Fiber: Oats, lentils, and vegetables help keep cholesterol in check.
-
Lean Proteins: Fish, chicken, or plant-based proteins are better than red meat.
-
Healthy Fats: Avocado, olive oil, and walnuts support heart health.
By combining these foods with a supervised fasting schedule, you can maximize the benefits while minimizing the risks to your heart.
FAQs (Frequently Asked Questions)
1. Can I take my heart medicine while fasting?
Most heart medicines can be taken on an empty stomach, but some require food to prevent side effects. You should never skip your medicine. Consult Dr. Ajay Bahadur, a Best Heart Doctor in Lucknow, to adjust your medication timing to fit your fasting schedule.
2. Is Intermittent Fasting (16:8) better than a 24-hour fast for the heart?
Yes. For heart patients, shorter fasting windows (like 12 to 16 hours) are much safer than long-term fasts. Long fasts increase the risk of electrolyte imbalances and dehydration, which can trigger heart rhythm problems.
3. Does fasting help clear blocked arteries?
Fasting can help reduce the risk factors that lead to blockages (like high cholesterol and inflammation). However, there is no medical evidence that fasting can “melt away” existing major blockages. Blocked arteries require medical treatment and lifestyle changes.
4. Can I exercise while fasting if I have a heart condition?
It is generally not recommended to do heavy exercise while fasting if you have heart disease. You may become dizzy or dehydrated. Light walking is usually fine, but always check with your cardiologist first.
5. What is the best way to break a fast for heart health?
The best way is to start with a small, balanced snack. Avoid high-carb, high-sugar, or high-salt foods. A bowl of vegetable soup or a few soaked almonds is a great way to wake up your digestive system without shocking your heart.
Conclusion
Fasting can be a powerful tool for health, but for heart patients, it is a double-edged sword. While it can help with weight loss and blood pressure, the risks of dehydration and mineral imbalance are real and dangerous.
The most important takeaway is this: Never fast alone. If you have a heart condition, your journey toward health must be guided by a medical professional. If you are looking for the best guidance, consulting a Heart Doctor in Lucknow – Dr Ajay Bahadur will ensure that your heart stays protected while you explore new ways to improve your well-being.
Your heart works hard for you every single second. Make sure you give it the fuel and care it needs, even when you are choosing to fast.
Disclaimer: This blog is for informational purposes only and does not substitute professional medical advice. Always consult your cardiologist before starting any new diet or fasting routine.


